Normal Development Of The Brain Across The Lifespan
To understand how traumatic stress occurring at different stages of the life cycle interacts with the developing brain, it is useful to review normal brain development. The normal human brain undergoes changes in structure and function across the lifespan from early childhood to late life. Understanding these normal developmental changes is critical for determining the difference between normal development and pathology, and how normal development and pathology interact.
Although the bulk of brain development occurs in utero, the brain continues to develop after birth. In the first 5 years of life there is an overall expansion of brain volume related to development of both gray matter and white matter structures however, from 7 to 17 years of age there is a progressive increase in white matter and decrease in gray matter while overall brain size stays the same.13–16 Gray matter areas that undergo the greatest increases throughout this latter developmental epoch include frontal cortex and parietal cortex.17,18 Basal ganglia decrease in size, while corpus callosum,19,20 hippocampus, and amygdala21–23 appear to increase in size during childhood, although there may be developmental sex-laterality effects for some of these structures.24 Overall brain size is 10% larger in boys than girls during childhood.24
Why Ptsd Affects Memory
“There are several theories surrounding why PTSD is associated with memory deficits,” Samuelson says. The first is that people with PTSD use so much of their energy in looking for threats and being hyper-attentive that they don’t have enough left over for thinking about the past. “Essentially, there is a cognitive burden of PTSD symptoms that taxes cognitive resources, pulling them away from memory and attention processes.”
The second theory is that the issues come from PTSD’s damaging effects on the brain. When somebody with PTSD is triggered, Samuelson says, the amygdala becomes over-activated and releases neurotransmitters that disrupt other brain areas, like the hippocampus and prefrontal cortex.
The third theory is that these deficits might not be a consequence of PTSD at all, but a potential risk. “A number of research studies have found that poorer cognitive functioning assessed prior to trauma served as a risk factor for the development of PTSD,” Samuelson says. “The flip side of that means that having strong memory abilities can play a role in protecting a person against developing PTSD.”
The reality, Samuelson says, is that all three are probably true. “There are preexisting deficits, there is a toxic effect of PTSD on memory, and finally, PTSD symptoms tax cognitive resources which in turn hinders a personâs ability to attend to, store, and recall information.”
Experts:
Kristin Samuelson Ph.D.
Studies cited:
How Does Trauma Affect The Brain
When we experience a traumatic event, our brain chemistry and functioning changes in response to the emotional and physical consequences of that event.
Traumatic events include a wide range of experiences, including:
- Physical or sexual abuse
- Death of a loved one
- Financial, professional, or personal loss
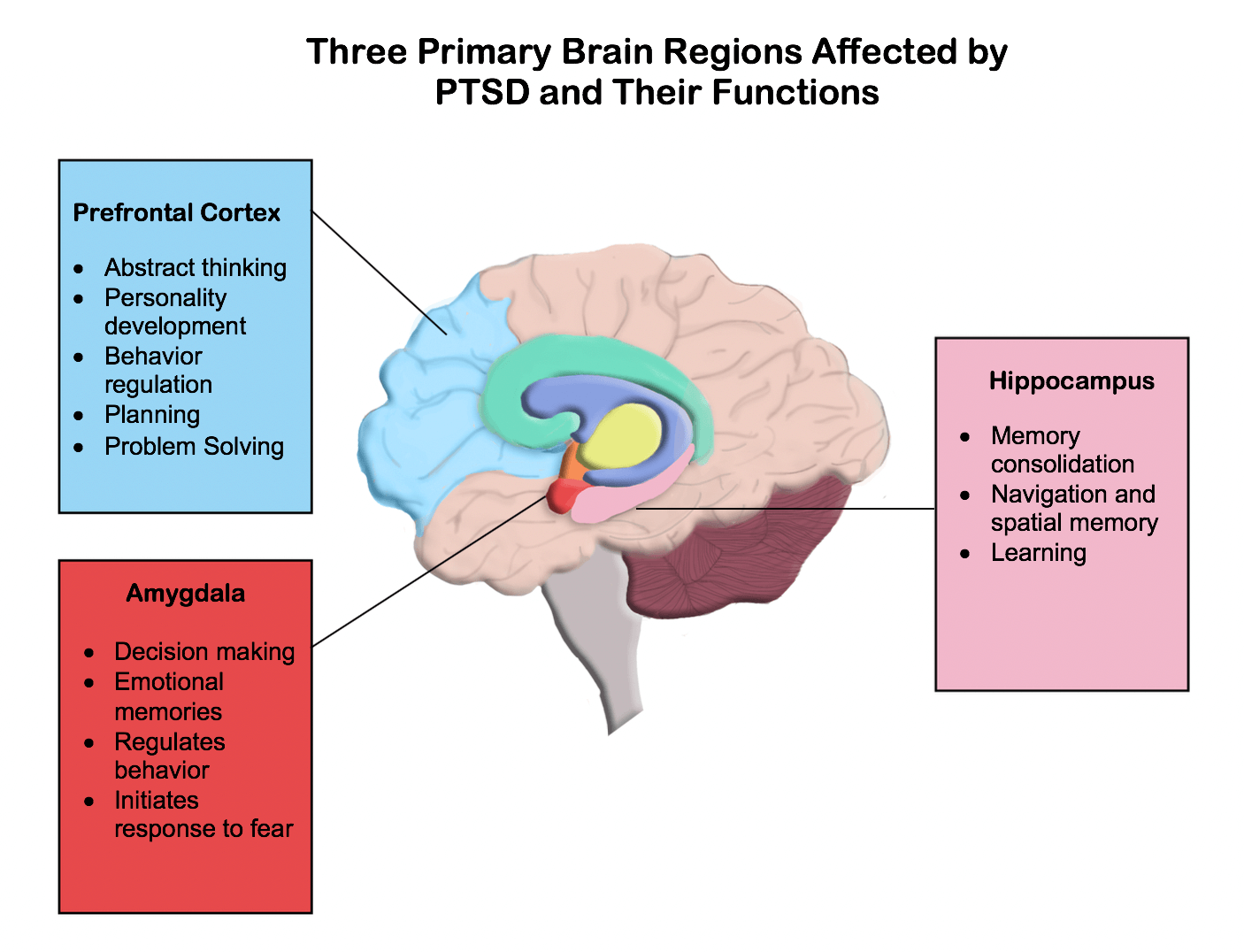
There is no standard definition of a traumatic experience for everyone, and each of these experiences takes a unique toll on us as individuals. While all of us experience traumatic stress in different ways, our brains process stress in mostly predictable patterns. In general, there are three major areas of our brain that are shaped by stressful experiences. These are:
- The hippocampus, which helps control memory, learning, and interpretation of information. This area of the brain may become less active under stress and, in fact, may actually shrink. This shrinkage reduces the amount of information and memories we can effectively process at one time. In addition, a smaller and less active hippocampus means we are less likely to be able to process any new information when we are experiencing traumatic stress.
- The amygdala, which helps us process our emotions. During periods of intense stress, the amygdalas role in the brain is to serve as an alarm system, alerting the rest of the brain to potential risk. While this is useful in life-or-death situations, the amygdala can be triggered by traumatic stress, too, causing the brain to enter fight-or-flight mode over and over again.
Read Also: How Much Can Someone Get On Disability
How Trauma Changes The Brain
After experiencing trauma, both the brain and the body react and change. Dr. Arkadiy Stolyar, Assistant Professor of Psychiatry, Harvard Medical School and Principal Investigator in Psychiatry at Boston Clinical Trials shares with us an article on how physical changes in the brain lead to symptoms of PTSD:
How Does Ptsd Happen
During a trauma, your body responds to a threat by going into âflight or fightâ mode. It releases stress hormones, like adrenaline and norepinephrine, to give you a burst of energy. Your heart beats faster. Your brain also puts some of its normal tasks, such as filing short-term memories, on pause.
PTSD causes your brain to get stuck in danger mode. Even after youâre no longer in danger, it stays on high alert. Your body continues to send out stress signals, which lead to PTSD symptoms. Studies show that the part of the brain that handles fear and emotion is more active in people with PTSD.
Over time, PTSD changes your brain. The area that controls your memory becomes smaller. Thatâs one reason experts recommend that you seek treatment early.
Don’t Miss: What Is Considered Short Term Disability
How This Information Can Be Used
There is still much to learn about the role certain parts of the brain play in PTSD formation. Knowing how PTSD affects the brain , however, is very important to study.
Understanding which parts of the brain may impact PTSD can lead to the development of more effective medications for treating the disorder. In addition, this information may also help us better identify who is at risk for developing PTSD following a traumatic event.
Brain Tissue Yields Clues To Causes Of Ptsd
A post-mortem analysis of brain tissue from people who had been diagnosed with post-traumatic stress disorder may help explain enduring mysteries about the disorder, such as why women are more susceptible to it and whether a dampened immune system response plays a role in dealing with stress, a team headed by Yale University and the VAs National Center for PTSD researchers has found.
The analysis of gene expression patterns in brain tissue located in four regions of the prefrontal cortex areas of the brain associated with higher cognitive function and executive control revealed distinct differences in those who had been diagnosed with PTSD and those who had not. Major differences in gene activity particularly affected two cell types in PTSD patients interneurons, which inhibit neural activity, and microglia, immune system cells in the central nervous system, the researchers report Dec. 21 in the journal Nature Neuroscience.
The findings suggest that together these changes might contribute to an impaired ability to respond to traumatic stress, said Matthew Girgenti, a research scientist in the Yale Department of Psychiatry and the NCPTSD and lead author of the study.
About half of PTSD patients are also diagnosed with some form of depression. However, gene expression patterns found in brain tissue are more closely linked biologically with schizophrenia and bipolar disorder than depression, the researchers found.
Related
Also Check: Can You Get Disability For Gout
Eye Movement Desensitization And Reprocessing
Eye movement desensitization and reprocessing is a technique that may help people with PTSD or complex PTSD.
After preparation and practice, the therapist will ask the person to recall the traumatic memory. The therapist will move a finger from side to side, and the person will follow the movement with their eyes.
When effective, this process helps to desensitize the person to the trauma so that they can eventually recall the memory without having a strong adverse reaction to it.
EMDR is controversial because the exact mechanism by which it works is unclear.
However, several guidelines, including those of the American Psychological Association, recommend EMDR as a treatment for PTSD under certain conditions.
They caution that confirming the effectiveness of EMDR for trauma will require more research.
How Common Is Post
Experiencing trauma is not rare as approximately 6 of every 10 men , and 5 of every 10 women will experience at least one traumatic event in their lifetime. Men are more likely to experience trauma in the form of accidents, physical assault, combat, or witness death or injury. Women are more likely to experience sexual assault and child sexual abuse.
Some people have inherited a gene from a parent who had PTSD, making them more susceptible to forming it themselves.
However, post-traumatic stress disorder can strike anyone at any time regardless of age or other demographics. No one is immune from PTSD, and as the world changes, it becomes more likely for one to experience a traumatic event that causes it.
Read Also: How Much Is Disability In Nj
Offer All Children In Care Targeted And Trauma
Children in care are likely to have experienced a complex mix of neglect, trauma and adversity. There is an urgent need to develop tailored interventions for the difficulties faced by these children. In the meantime, all children in care should be offered interventions based on the best current evidence, and that target trauma symptoms and cognitive skills.
Targeted strategies include:
- Trauma-Focused CBT
- Dialectical Behaviour Therapy and
- interventions that focus on the development of specific cognitive skills .
At present, Trauma-Focused CBT is the approach that has most empirical support . This trauma-specific intervention has also been shown to improve broad aspects of executive functioning such as cognitive skills and emotional regulation . Therefore, until more tailored interventions are developed for the complex needs of children in care, trauma-specific therapy should be offered as part of the support plan for children who have been exposed to traumatic events. Ideally, this input will occur in the context of a trauma- aware organisational framework .
Emotion Trauma And The Prefrontal Cortex
The ventromedial prefrontal cortex is a part of the brain that regulates emotions. This emotion-regulating center is often affected after trauma and becomes vulnerable to other parts of the brain.
Normally, the amygdala will sense a negative emotion, such as fear, and the prefrontal cortex will rationally react to this emotion. After trauma though, this rationality might be overridden and your prefrontal cortex will have a hard time regulating fear and other emotions.
So, these three parts of the brain- the amygdala, the hippocampus, and the prefrontal cortex- are the most-affected areas of the brain from trauma.
They can make a trauma survivor constantly fearful, especially when triggered by events and situations that remind them of their past trauma.
Overcoming emotional trauma is a long process, but it is possible. If you are suffering from after-effects of emotional trauma or PTSD, know that recovering from your trauma is possible.
Don’t Miss: Is Post Traumatic Stress Disorder A Disability Uk
Develop And Support Positive Relationships And Connections In Children’s Lives
Any placement of a traumatised child should ensure the child’s safety and connect him or her to positive influences and relationships in the home, school, and broader community. Positive family functioning, safe living environments and positive relationships in school and community are likely to facilitate cognitive development.
Special attention may be needed to maximise the positive aspects of family contact or to protect the child from ongoing exposure to trauma via family contact. Supporting placement stability will ensure continuity of relationships and a necessary foundation for recovery by facilitating predictability and safety. Ensuring placement stability will increase the likelihood that there is a person that is available who understands well the impact of trauma on the child.
This caregiver can help the child, the child’s statutory caseworker and other significant players to make sense of how trauma and adversity has affected the child, and what is needed to move forward. Interventions with young children in care demonstrate that continuous, consistent and responsive caregiving can change brain stress hormone levels and improve their capacity for self-regulation .
% Commission In Real Estate

You may have heard or read about the term 100% commission with regard to real estate. It has to do with the commission split an agent makes who is selling or listing a property.
Typically, real estate agents work for a large firm such as ReMax or Coldwell Banker, which provide shared office space, supplies, utilities, and more in exchange for monthly dues and a split of the commission.
In other words, that 2.5% or 3% commission doesnt all go to the agent. Instead, a portion goes to the broker for providing support along the way.
Read Also: How Much Does Ssi Disability Pay
Provide Safe Environments And Rich Experiences That Stimulate And Enrich Brain Growth
Cognitive development will be supported by stable caregiving. Continuous and nurturing caregiving will support brain development by fostering psychological safety. The experience of psychological safety reduces the need to be engaged in constant vigilance, enabling children to make the most of learning and development opportunities. There are often barriers to children in care experiencing psychological safety. It is important not to equate physical safety with psychological safety, which may take time to develop. Children may not experience psychological safety when first placed in care due to belief that adults are dangerous. Out-of-home care environments may also inadvertently undermine psychological safety . Children placed with people whose behaviour is frightening or dangerous may not experience the necessary psychological safety, and their capacity for new learning will be diminished.
The Brain Changes Caused By Trauma
While alterations in behavior are the hallmarks of PTSD, the causes for these changes involve changes to significant brain structures. One study using functional magnetic resonance imaging showed that brain structure and function might underlie the symptoms of post-traumatic stress disorder.
The brain areas that seem to have been consistently implicated in PTSD have included the hippocampus and the prefrontal cortex . Also involved in the changes seen in those living with PTSD is the amygdala .
Several studies have shown that PTSD is associated with a reduction in the hippocampus volume during fMRI and MRI examinations. This volume change can mean that the person experiencing post-traumatic stress disorder will experience memory disturbances and difficulty learning.
The amygdala volume in people with PTSD decreased, leaving the person living with PTSD easily triggered by events it perceives as dangerous, whether this perception is correct or not. As a result, the person lives in a state of constant alertness and fear and can be easily triggered into a flashback of the event that caused their post-traumatic stress disorder .
Also Check: How To Apply For Short Term Disability In Texas
How Psychological Trauma Effect On The Brain
People that experience trauma not only suffers from mental health issues such as depression and anxiety, they may even have significant effects of trauma on the brain. Victims of trauma, particularly those who develop PTSD may have their brain rewired in a sense due to their exposure to trauma. Childhood trauma can even impact the developing brain and cause variations in the volume and function of the brain.
Researchers are continuing to determine exactly how PTSD impacts and even the effect of trauma on the brain that doesnt result in PTSD. Understanding how trauma affects the brain may help create new treatment methods to help reduce and minimize some of the painful emotional symptoms associated with trauma. PTSD symptoms can be frightening and debilitating so gaining insight into how the brain functions differently may be useful in recovery.
Tools like neuroimaging are used to create maps of the brain in order to study PTSD sufferers. These maps show areas of the brain that vary from normal non-trauma brain structure. Traumatic stress leads to significant changes in brain structure and function that cause the victim to continue experiencing stress.
Factors Supporting Children’s Development Following Trauma And Adversity
The following section outlines six principles that might be useful in supporting the development of cognitive skills in children who have been exposed to trauma and other adversity. These principles are based on conclusions drawn from current theory and empirical research.
There is relatively little research on interventions to support the recovery of cognitive skills in children affected by trauma and adversity . Studies have only just begun to include improvements in cognitive skills as part of outcome measurement . As a result our knowledge is limited, although this is an emerging field of research.
The National Child Traumatic Stress Network and Blue Knot have produced practice guidelines for addressing trauma that emphasise the importance of:
- providing physical and psychological safety for the child
- supporting safe, positive and stable relationships
- supporting the child to develop emotional regulation skills and
- enlisting coordinated support and self-care for personal and professional stress.
The guidelines are useful for supporting recovery of traumatised children, but they do not necessarily address the other needs that children in out-of-home care might have.
Don’t Miss: How Much Do You Get On A Disability Pension
How Does Ptsd Affect The Body
Looking again at our natural preparation in times of stress and danger, the biochemical stress response also readies our bodies for survival by increasing the heart rate and circulation, increasing glucose in the blood for energy, and slowing digestive, reproductive, and immune systems since they are secondary for survival. We are prepared to fight or to flee when faced with real danger. But sometimes this stress response fires even when real danger is not present. And this is very common for someone with a trauma disorder who has not had the opportunity to process their past traumatic experiences in a supportive recovery environment.
We are not meant to have the brains stress centers firing so often as they do in the context of post-traumatic stress disorder. Not only does an overactive stress response tax the brain, emotions, and memory it also puts dangerous strain on the body. The following physical conditions have been associated with PTSD:
- Heart disease
- Weakened immune system
