What Is The Prognosis For People With Traumatic Brain Injuries
Recovery from a TBI is highly individualized. It depends on the severity, cause and type of injury. People with mild TBIs are expected to improve and return to their pre-injury functioning within days to a few months. Some people with mild TBIs have few concerns and never seek treatment.
Moderate to severe TBIs can cause more significant difficulties with changes to their thinking and behavior. People with severe TBIs can have lifelong changes.
There are several different factors that can influence someones recovery.
Tbi And Ptsd: Similarities And Differences
Synopsis:For someone living with a diagnosis of both TBI and PTSD the combination can be overpowering and destructive. While awareness of PTSD has increased greatly with recently returning service members and veterans, it is not new or limited to combat. One estimate suggests up to 35% of returning veterans with a mild brain injury also experience PTSD.
Tbi Ptsd And Substance Abuse
The effects of alcohol are magnified following a brain injury. Consuming alcohol:
- Slows reactions
- Increases the risks of seizures
- Increases the risk for another brain injury
The only safe amount of alcohol following a brain injury is – None. Where PTSD is concerned, using alcohol and drugs to self-medicate is dangerous. Veterans who drink more heavily and binge drink more often than civilian peers are at increased risk. Alcohol and drugs are being used often by veterans to cope with and dull the symptoms of PTSD and depression. The fact is, alcohol and drug use creates additional issues with thinking, memory and behavior.
Read Also: Does Degenerative Disc Disease Qualify For Disability
How Tbi Differs From Ptsd
The difference with TBI is in how the brain thinks, learns, and the ways a person can function differently than with PTSD. The brain is very complex with the possible effects of a traumatic injury that are different for each person. When PTSD and TBI coexist, it is difficult to know what is happening. Changes in cognition like memory, depression, and fatigue are common with both diagnoses. A person basically feeds and reinforces the other so it makes things really complicated. Some other key differences may include:
- A period of amnesia just before or after the injury occurred is common. Before a crash, explosion, or other incidents that cause the TBI, a person may not remember some of the events leading up to or immediately following it
- PTSD is often associated with haunting, intrustive thoughts and memories of what happened as if the person relives it day in and day out
- Sleep disorders can happen frequently with TBI, including waking early, difficulty staying asleep, or disruption to normal sleep patterns
- Survivors of TBI really support visits of friends and coworkers change over time. Social isolation can feel difficult, even for people with PTSD who experience similar issues
- Cognitive fatigue is a big issue with brain injury. Thinking and learning become harder. Emotions are unpredictable and a person may not know how to respond emotionally
Diagnosis And Assessment Of Traumatic Brain Injury
This chapter provides an overview of traumatic brain injury , including how it is defined, its mechanisms of injury, and its neuropathology. The chapter also provides a conceptual model on the recovery trajectories after TBI and intrinsic factors related to the variability in its presentation and diagnosis and in recovery from TBI. There is a discussion of the complexity of establishing a diagnosis of TBI, especially mild TBI , the role of neuroimaging after injury, and the limitations of the current approaches. Finally, there is a discussion of which health care providers are qualified to make the diagnosis as well as the additional complexity of common co-occurring conditions in diagnosing TBI.
You May Like: What Is Social Justice In Disability
Emerging Evidence On Natural History Of Mild Tbi
While considerable research has been conducted on mTBI, the diagnosis of mTBI and the prognosis offered after a finding of mTBI continue to be complicated and sometimes controversial. However, it is likely that three ongoing, large-scale, multi-center, observational, longitudinal studies that are now in the advanced stages of data collection, curation, and analysis will reveal new information about both the psychosocial and neurobiologic manifestations of mTBI.
The Chronic Effects of Neurotrauma Consortium was established in 2013 via a federal cooperative agreement responding to the National Research Action Plan for improved prevention, diagnosis, and treatment of service members and U.S. veterans with TBI. The centerpiece of CENC is a multicenter, longitudinal, observational study designed to address gaps in knowledge about who served in Operation Iraqi Freedom and Operation Enduring Freedom and experienced mTBI. Data are being collected from more than 30 academic universities, 15 VA medical centers, and 3 military treatment facilities. The study’s overarching goal is to understand the associations among chronic effects of mTBI, neurodegenerative disorders, and common comorbidities, including psychological, neurologic , sensory , movement, pain , and cognitive and neuroendocrine disorders. CENC will collect data and conduct annual follow-up interviews on the research participants.
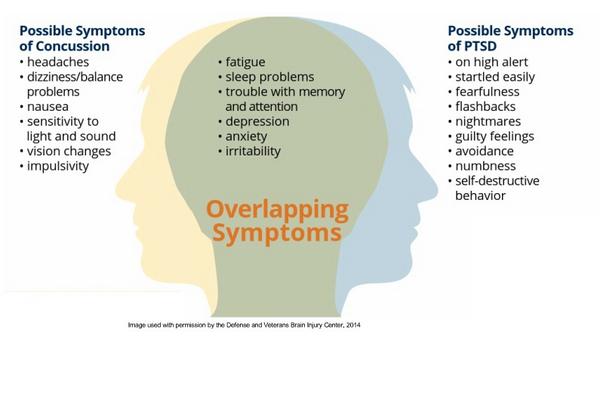
Postconcussive Syndrome And Ptsd
The issue of postconcussive syndrome is a vexed one, both in terms of its definition and its purported causes. It is also an issue that intersects with symptoms of PTSD. PCS is generally defined as a syndrome that involves headache, dizziness, fatigue, sensitivity to light or sound, sleep disturbance, and concentration difficulties.93 The definitions of PCS vary, and generally overlap somewhat with symptoms of PTSD. For example, the International Classification of Diseases 26 stipulates that PCS is defined by headaches, dizziness, general malaise, fatigue, noise intolerance, irritability, emotional lability, depression, or anxiety, concentration or memory difficulty, sleep disturbance, reduced tolerance to alcohol, and a preoccupation with these symptoms and fear of permanent brain damage. The Appendix of the DSM.-IV4 describes PCS as fatigue, sleep disturbance, headaches, dizziness, irritability, anxiety or depression, changes in personality, and apathy. These descriptions clearly overlap with common symptoms of post-traumatic stress, and represent differential diagnosis problems insofar as how one attributes these symptoms to PCS or PTSD.
Don’t Miss: How To Ask Your Doctor For Short Term Disability
How Do They Cause Cognitive Issues
Until recently, researchers didnt understand exactly what these conditions were doing in the brain, and in particular how they affected cognition.
According to this review, TBI and PTSD represent brain disorders with disruptions in neural networks that communicate via long axonal pathways through white matter tracts, termed the connectome. The connectome is the brains wiring pattern the sum total of billions of neurons and the pathways or routes that they use to carry out their function.
Both TBI and PTSD have shown to produce neural inflammation, excitotoxicity, and oxidative stress within the brain. These processes, all of which can affect one another, represent normal functions in the body that, under every day conditions, dont cause harm. If these functions get pressed into service too often or for too long though, they can kick into overdrive and quickly spiral out of control, leading to cellular damage and physical changes in the brain.
For example, the amygdala is largely responsible for the raw data of emotions that arise in the body. But its your prefrontal cortex that actually works with the amygdala to regulate emotions. Studies have shown that a critical connection between the prefrontal cortex and amygdala may be broken in brains with TBI or PTSD, which could explain the commonly seen lack of emotional control.
How Is A Traumatic Brain Injury Diagnosed
Your healthcare provider will examine you and ask about your symptoms. They will also want to learn more about what caused the injury. Depending on the severity of the injury and symptoms, you may have:
- Neurological evaluation: A neurologist checks your memory, thinking, motor function and sensory functions .
- Imaging tests: A CT scan or MRI checks for brain bleeding and swelling.
- Blood test: The Banyan Brain Trauma Indicator looks for proteins in your blood that indicate concussion or mild TBI.
You May Like: Who Is The Best Social Security Disability Lawyer
What Causes A Traumatic Brain Injury
When you take a violent, hard hit to your head, your brain may experience changes in chemical and energy use as a way to compensate for the injury. These changes can result in headaches, light/sound sensitivity, and confusion. In mild TBIs, these changes are short and do not permanently damage the brain. However, with more severe injuries, these changes can last longer and result in damage to the brain cells. These effects can cause the brain to swell and expand inside the skull. The swelling can lead to even more brain damage.
What Are The Complications Of A Traumatic Brain Injury
A moderate or severe TBI can cause permanent brain damage and disabilities. People with TBIs also have a higher risk of:
- Seizures .
In rare cases, severe head injuries or having had several moderate to severe TBIs can increase someones risk to developing Alzheimers disease, dementia, or movement disorders later in life. Reassuringly, this is unlikely to happen with a mild TBI.
Finally, chronic traumatic encephalopathy or CTE can occur. This is a condition that happens when someone has had several blows to the head over an extended period, such as professional athletes. This condition is in the early stages of research and is still in the process of being understood. Currently, this condition cannot be diagnosed until the brain tissue at autopsy.
Don’t Miss: How Does Social Security Disability Work When A Spouse Dies
Study Highlights Challenges In Diagnosis Treatment In Veterans And General Population
byElizabeth Hlavinka, Staff Writer, MedPage Today October 29, 2018
AUSTIN, Texas — Malingering should be considered when diagnosing post-traumatic stress disorder and traumatic brain injury in certain situations such as forensic settings, according to a review of current data.
Since PTSD and TBI have similar symptoms and are both most commonly diagnosed in veterans, it may be increasingly difficult to distinguish between the two, particularly since anywhere from 6% to 44% of those with TBI also have PTSD, reported Jeffrey Guina, MD, a forensic psychiatrist in Michigan.
The DSM-5 defines malingering as “intentional production of false or grossly exaggerated physical or psychological symptoms, motivated by external incentives such as avoiding military duty, avoiding work, obtaining financial compensation, evading criminal prosecution, or obtaining drugs.”
TBI and PTSD may be differentially incentivized in private and veteran’s affairs disability systems, which may lead to false reports, Guina and colleagues explained in a poster at the American Academy of Psychiatry and the Law meeting.
While PTSD generally results from past trauma, and TBI often follows a physical brain injury such as direct force, a blast injury, or diffuse axonal shearing, both can have similar fMRI findings, particularly within the dorsolateral prefrontal, orbitofrontal, medial frontal, and anterior cingulate cortices, Guina reported.
Disclosures
First Things First: Pcs Treatment
When a person sustains a mild traumatic brain injury, they often experience inflammation and sometimes swelling. As the brain tries to cope with that inflammation and other issues caused by the head injury, it may establish workaround communication pathways to bypass injured parts of the brain.
Unfortunately, these detours arent as efficient as the original pathways the brain tires quickly while using them, leading to post-concussion symptoms. When the brain continues to use these inefficient pathways even after the initial injury resolves, the symptoms persist indefinitely.
We have developed a highly effective treatment for post-concussion symptoms using the brains inherent ability to repair itself to encourage the brain to return to using its efficient, pre-injury pathways.
Epic Treatment takes place during an intense week at our facility. It begins with a functional Neurocognitive Imaging Scan that allows us to look at how a patients brain is responding to a series of cognitive demands. We measure the blood flow to specific regions, looking for areas of dysfunction. We then use the fNCI results and an inventory of the patients symptoms to create an individualized treatment plan that targets those dysfunctional brain regions.
Though many patients show remarkable improvement during treatment week, patients are given instructions on how to continue treatment at home. This is a vital part of the recovery process.
Also Check: Social Security Office In Des Moines Iowa
Characteristics Of The Two Groups
Characteristics of the two groups are presented in Table . Five of the total sample of 46 patients were diagnosed with PTSD . Only one out of the five PTSD-patients had been unconscious at the time of the accident, all the others had been conscious. Table also shows the proportion of PTSD for the two groups. The difference is significant according to Fisher’s exact P-value.
Table 1 Characteristics for the two groups .
Why Does Depression Occur Alongside Anxiety Adhd Ptsd Or Tbi So Often
There is one important link that connects depression to other conditions like anxiety, ADHD, PTSD, and TBIthe frontal lobe of the brain. The frontal lobe is involved in numerous functions relating to mood, including self-awareness, personality, attention, memory, and moral and social reasoning.
In the case of depression and anxiety, researchers believe that an imbalance in activity in the left and right frontal lobes causes these two conditions to occur at the same time. When the right lobe is overactive, it can lead to symptoms associated with both depression and anxiety, like withdrawing and being defensive.
You May Like: How Far Back Can Social Security Go For Overpayment
Tbi And Ptsd: Navigating The Perfect Storm
So often people talk about the effects of traumatic brain injury or the consequences of post-traumatic stress disorder as separate conditions which they are. But for the person who is living with the dual diagnosis of TBI and PTSD, it can be hard to separate them.
Just as meteorologists predict the perfect storm when unusual and unprecedented conditions move in to create catastrophic atmospheric events, so can the combination of PTSD and TBI be overpowering and destructive for all in its path. The person with TBI and PTSD is living in a state unlike anything previously experienced. For the family, home is no longer the safe haven but an unfamiliar front with unpredictable and sometimes frightening currents and events.
While awareness of PTSD has greatly increased with recently returning service members and veterans, it is not new and nor limited to combat. Anyone children, adolescents, adults, elderly who is exposed to a life-threatening trauma can develop PTSD. Car crashes, shootings, floods, fires, assaults, or kidnapping can happen to anyone anywhere. But the rate of PTSD after brain injury is much higher in veterans than civilians due to their multiple and prolonged exposure to combat. According to OConnor and Drebing, it is estimated that up to 35% of returning veterans with mild brain injury also have PTSD.
How Serious Is My Injury
A TBI is basically the same thing as a concussion. A TBI can be mild, moderate, or severe. These terms tell you the nature of the injury itself. They do not tell you what symptoms you may have or how severe the symptoms will be.
A TBI can occur even when there is no direct contact to the head. For example, when a person suffers whiplash, the brain may be shaken within the skull. This damage can cause bleeding between the brain and skull. Bruises can form where the brain hits the skull. Like bruises on other parts of the body, for mild injuries these will heal with time.
About 80% of all TBI’s in civilians are mild . Most people who have a mTBI will be back to normal by three months without any special treatment. Even patients with moderate or severe TBI can make remarkable recoveries.
The length of time that a person is unconscious is one way to measure how severe the injury was. If you weren’t knocked out at all or if you were out for less than 30 minutes, your TBI was most likely minor or mild. If you were knocked out for more than 30 minutes but less than six hours, your TBI was most likely moderate.
You May Like: How To Get A Disability Dog
More Fda Actions And Research On Tbi
The FDA continues to work with the research and clinical community to develop better-designed clinical studies so new medical products can be developed. And the FDA continues to review and evaluate medical devices for safety and effectiveness.
More sensitive and objective ways to diagnose and detect mild TBI are needed. Timely diagnosis is important to prevent repetitive injury and to help develop new therapies. Thats because repetitive injury carries the risk of second impact syndrome. If people who have not recovered from a head injury have a second head injury, this can result in more significant injury to the brain and more neurological deficits. And, in some cases, repetitive injury can be fatal or cause dementia later in life.
The FDAs scientists continue to conduct research on diagnostic tests for mild TBI. The scientists are studying TBI blood tests, special brain imaging, eye movements, and brain wave patterns. They are also investigating using portable imaging devices to detect mild TBI.
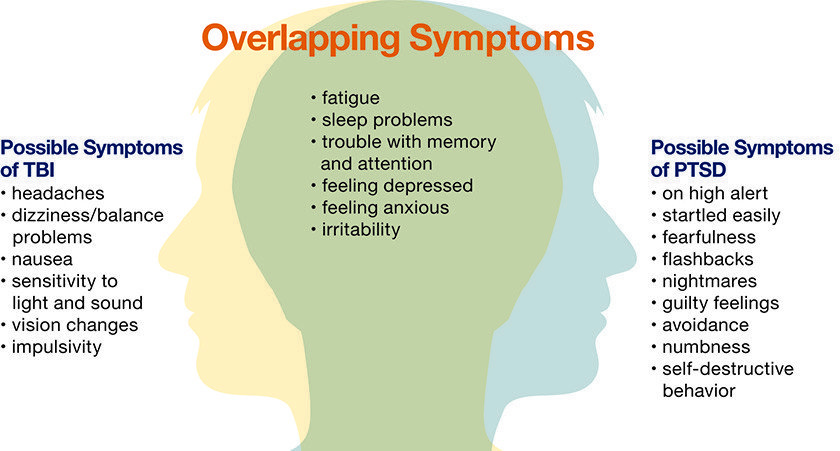
Diagnosing Ptsd Symptoms After Traumatic Brain Injury
PTSD and traumatic brain injury share many characteristics. Unfortunately, this can make determining the origin of a persons symptoms quite difficult. Some common symptoms the two share include headaches, light and noise sensitivity, difficulty concentrating, anxiety, and insomnia, among other side effects.
However there are a few symptoms that are more unique and indicative of PTSD. These include:
- Involuntary recurring thoughts of the life-threatening event
- Avoiding people and places that remind you of your injury
- Emotional numbness and feeling detached from friends and family
- Overwhelming feelings of shame and guilt
- Hypervigilance, i.e. constantly feeling on your guard, irritable, or easily startled
- Angry outbursts or aggressive behavior
While some of these symptoms can also overlap with TBI , what distinguishes PTSD from ordinary brain injury symptoms is feeling immobilized by them.
In other words, you cant ignore these feelings, they are interfering with your daily life, and you are unable to move forward. You feel stuck, like your feet are sinking in quicksand. That is PTSD.
Additionally, the symptoms of PTSD can last for months or years. While some remaining deficits from TBI can last a long time as well, the intensity of the emotional and behavioral symptoms should begin to fade after a few months.
Don’t Miss: How Much Is Disability In Ny
