Exposure To Ptes And Probable Ptsd Diagnosis
Responses on the HTQ revealed that participants in this sample had been exposed to multiple types of PTEs. On average, participants had experienced 5.68 types of PTEs, with the vast majority reporting exposure to at least one type of PTE. The frequency of exposure to PTEs are summarised in Table . Participants most commonly experienced lack of food or water and being close to death . Additionally, more than one third of the sample had experienced imprisonment and/or torture , and just under one fifth were survivors of rape or sexual abuse . A total of 51 participants were identified as having a probable diagnosis of PTSD.
Table 3 Frequency of Exposure to Potentially Traumatic Events
Ptsd With Dissociative Features
- With dissociative symptoms . :272, :1145
- All the PTSD criteria are met
- “High levels of depersonalization or derealization” are also present
- Dissociative symptoms are not linked to substance use or another medical condition
- it is found in both children and adults
What Is The Dsm
Used to diagnose mental disorders, DSM stands for Diagnostic and Statistical Manual of Mental Disorders. It’s a book that is basically like an encyclopedia of psychological disorders. The book originally was published in 1952, but has been updated multiple times resulting in the current edition of the DSM-5.
The DSM was created by over a hundred and sixty clinicians and researchers from all over the globe. The purpose of creating the DSM is to provide a handbook for mental health professionals and other healthcare workers.
The DSM includes lists of symptoms and criteria that they can use in order to diagnose patients with mental disorders. This guidebook helps to make diagnosis and communication about mental illness more consistent.
Over the years, the book has continued to be updated and revised as there is research consistently happening on an ongoing basis around mental health disorders. These revisions help to keep the book accurate for our current day in order to help the most amounts of people. The most recent additions to the book were made in order to include symptoms that people were commonly experiencing with mental disorders such as PTSD, but we’re not already included in the book.
Read Also: How To Apply For Disability In Missouri
Prevention And Early Intervention
- Meta-analyses currently do not support the widespread use of individual psychological debriefing in reducing the intensity of PTSD symptoms.
- The evidence for group debriefings is unclear at this time, and is still commonly done in first-responder settings .
- Multisession trauma-focused cognitive behavioural therapy can be helpful for individuals with PTSD or acute stress disorder.
- Thus, screening for and treating appropriate individuals is recommended over debriefing all trauma victims.
PsychDB is an Amazon Associate and earns from qualifying purchases. Thank you for supporting our site!
What Are The Implications Of The Dsm
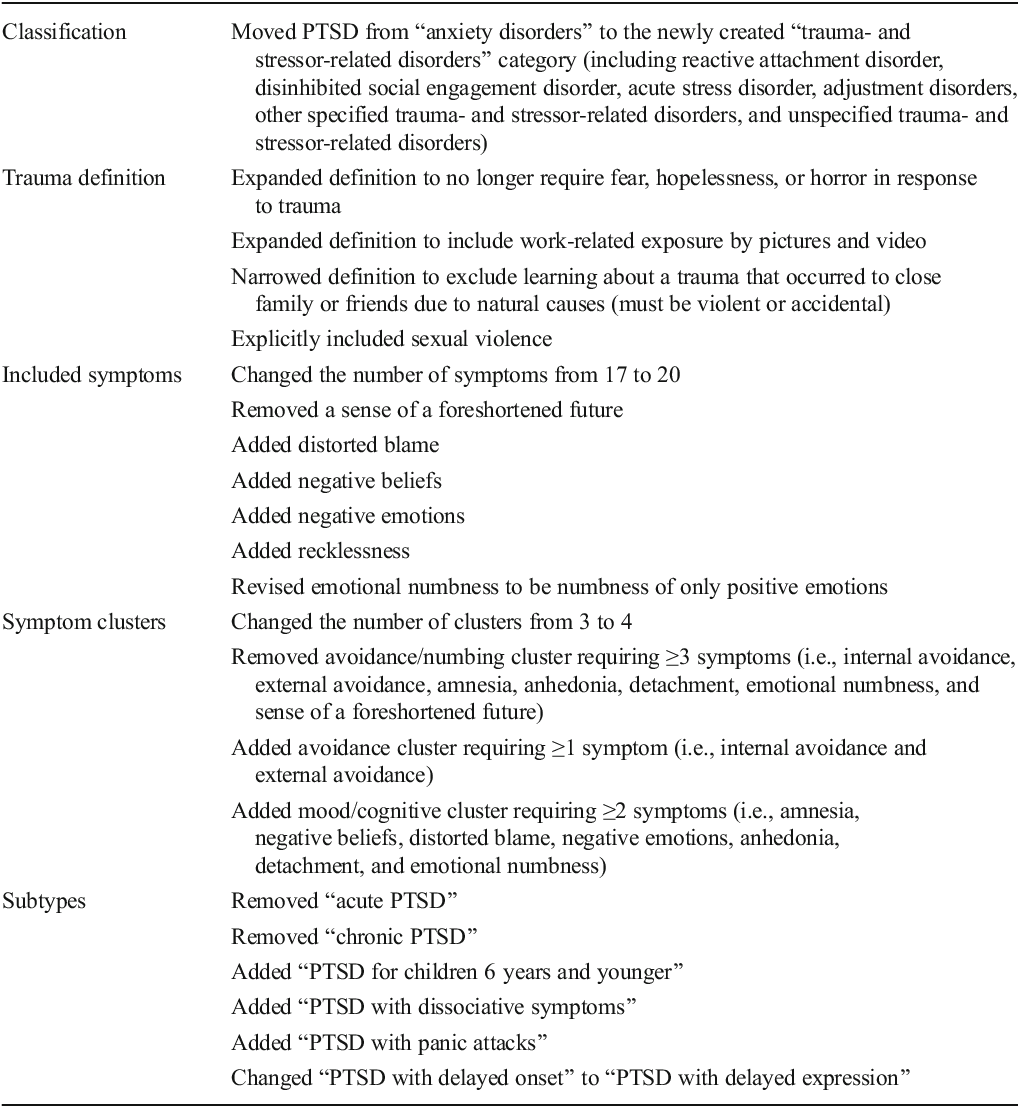

Changes in the diagnostic criteria have minimal impact on prevalence. National estimates of PTSD prevalence suggest that DSM-5 rates were only slightly lower than DSM-IV for both lifetime and past-12 month . When cases met criteria for DSM-IV, but not DSM-5, this was primarily due the revision excluding sudden unexpected death of a loved one from Criterion A in the DSM-5. The other reason was a failure to have one avoidance symptom. When cases met criteria for DSM-5, but not DSM-IV, this was primarily due to not meeting DSM-IV avoidance/numbing and/or arousal criteria . Research also suggests that similarly to DSM-IV, prevalence of PTSD for DSM-5 was higher among women than men, and increased with multiple traumatic event exposure .
Also Check: How To Get Disability For Multiple Sclerosis
Other Changes To Ptsd Diagnosis
Another change is sub-dividing Criterion C. In the DSM-IV, Criterion C included avoidance and numbing. The DSM-5 subdivides those into Criterion C and Criterion D. Criterion C is avoidance and Criterion D is negative alterations in cognitions and mood. This subdivision more clearly defines the behavior that PTSD sufferers manifest according to clinical evidence. For example, the new Criterion D specifically lists what is commonly called survivor guilt. The DSM-5 describes this as persistent distorted blame of self or others for causing the traumatic event or for resulting consequences. This is entirely new language that is not present in the DSM-IV.
Another change from sub-dividing the DSM-IV Criteria C is that the sheer number of Criterion C elements has been reduced. The new Criterion C language in the DSM-5 is much simpler:
- Persistent effortful avoidance of distressing trauma-related stimuli after the event
- Trauma-related thoughts or feelings
- Trauma-related external reminders
This simplification is consistent with the DSM-5s emphasis on behavior negative alterations in cognitions and mood, Criterion D. The number of elements needed from Criterion D has remained the same: two.
Criterion B: Intrusion Symptoms
The traumatic event is persistently re-experienced in the following way:
Read Also: Is My Va Disability Compensation Taxable
Specify If: With Dissociative Symptoms
In addition to meeting criteria for diagnosis, an individual experiences high levels of either of the following in reaction to trauma-related stimuli:
Criterion D: Physical Reactivity
The individual must also exhibit at least two of the following negative changes in mood or cognition.
- Cannot remember details about the event
- Persistent, negative beliefs about themselves, others, or the world as a whole
- Blaming oneself for the events occurrence
- Persistent negative emotional state, for example sad, angry, fearful
- Feeling detached from others
- Inability to experience positive emotions
You May Like: Do Pensions Affect Social Security Disability Payments
Disinhibited Social Engagement Disorder
Disinhibited social engagement disorder occurs in children who have experienced severe social neglect or deprivation before the age of 2. Similar to reactive attachment disorder, it can occur when children lack the basic emotional needs for comfort, stimulation and affection, or when repeated changes in caregivers prevent them from forming stable attachments.
Disinhibited social engagement disorder involves a child engaging in overly familiar or culturally inappropriate behavior with unfamiliar adults. For example, the child may be willing to go off with an unfamiliar adult with minimal or no hesitation. These behaviors cause problems in the childs ability to relate to adults and peers. Moving the child to a normal caregiving environment improves the symptoms. However, even after placement in a positive environment, some children continue to have symptoms through adolescence. Developmental delays, especially cognitive and language delays, may co-occur along with the disorder.
The prevalence of disinhibited social engagement disorder is unknown, but it is thought to be rare. Most severely neglected children do not develop the disorder. Treatment involves the child and family working with a therapist to strengthen their relationship.
What Is Acute Stress Disorder
UK health organisationMSD defines Acute Stress Disorder as an intense, unpleasant, and dysfunctional reaction beginning shortly after an overwhelming traumatic event and lasting less than a month. If symptoms persist longer than a month, people are diagnosed as having posttraumatic stress disorder . As you can see from this definition, Acute Stress Disorder and PTSD share a few similarities in that both conditions are different from the simple and routine exposure to stress that most people experience on a daily basis.
To put this difference into a practical context, lets consider two different scenarios. For example, imagine that your daily commute to and from work is routinely clogged with traffic. Every time you leave for work or head home, it seems as though your entire city has come out onto the highway! As a result, your commute may take 30 minutes longer than it should and you might feel irritable and frustrated. But even if you feel that frustration every day, youre unlikely to develop Acute Stress Disorder as a result.
People with this disorder may have dissociative symptoms. For example, they may feel emotionally numb or disconnected from themselves. They may feel that they are not real. The number of people with acute stress disorder is unknown. The likelihood of developing acute stress disorder is greater when traumatic events are severe or recurrent.
Symptoms of Acute Stress Disorder are very similar to symptoms of PTSD and can include:
Medication
You May Like: Complex Ptsd: From Surviving To Thriving
New Dsm Category For Trauma And Stressor
So what is different about the disorders in the new category? The DSM-5 differentiates the disorders in the category using different combinations of specific symptoms: expression of anxiety, externalizing anger or aggression, levels of depressive symptoms, and dissociative events. This is important, because it could mean that veterans who do not receive a diagnosis for PTSD may, in fact, suffer from some other kind of trauma and stressor-related disorder that the VA could service connect. Veterans and advocates should read the entire list of disorders in the trauma and stressor related disorders category and keep this list in mind when reviewing medical records.
Ptsd Illusions And Hallucinations
hearing voicesParanoia
“Flashbacks in Posttraumatic Stress Disorder must be distinguished from illusions, hallucinations, and other perceptual disturbances that may occur in Schizophrenia, other Psychotic Disorders, Mood Disorder with Psychotic features, a delirium, Substance-Induced Disorders, and Psychotic Disorders Due to a General Medical Condition.” :467
Recommended Reading: Where Can I Get The Disability Forms
Ptsd In Preschool Children
Infants and children aged six years old or younger can be diagnosed with PTSD, but young children’s thinking and ability to express themselves in words is limited. This means both their symptoms and diagnostic criteria are slightly different from those in adults or older children. Most of the research on Preschool PTSD involved three- to six-year-olds, with some studies also including younger children. Babies and toddlers can have PTSD: the minimum age for diagnosis is one year old.:272-274The criteria for Posttraumatic Stress Disorder for Children 6 Years and Younger are “developmentally sensitive”. Some of the changes from the main PTSD criteria include:
- constricted play is an example of “diminished interest in significant activities”
- social withdrawal or behavioral changes can indicate “feelings of detachment or estrangement.
- extreme temper tantrums are now included with “irritability or outbursts of anger”
- intrusive symptoms such as flashbacks and intrusive thoughts do not always manifest overt distress in preschool childrenScheeringa states that “while distressed reactions are common, parents also commonly reported no affect or what appeared to be excitement”
- fewer avoidance symptoms are included because avoidance is internalized, and harder to detect by observation, for example in pre-verbal children
Developmental Trauma Disorder
What Is The Definition Of Trauma
Trauma is an emotional or physical response to one or more physically harmful or life threatening events or circumstances with lasting adverse effects on your mental and physical well-being, according to the Substance Abuse and Mental Health Services Administration .
This could be an event youve personally experienced, witnessed happening to someone else, heard about happening to a close loved one, or heard about through your job .
For more information and support tools, you can read Psych Centrals Finding a Path Through Trauma resource.
The symptoms of PTSD fall into four main groups:
- intrusion symptoms
- changes in cognition and mood
- physical reactivity
After a traumatic event, you may experience at least one of these intrusion symptoms:
- intrusive memories about what happened
- distress when youre reminded of the incident
- physical reactions to stress, like increased heart rate and blood pressure
You May Like: Is Cerebral Palsy A Developmental Disability
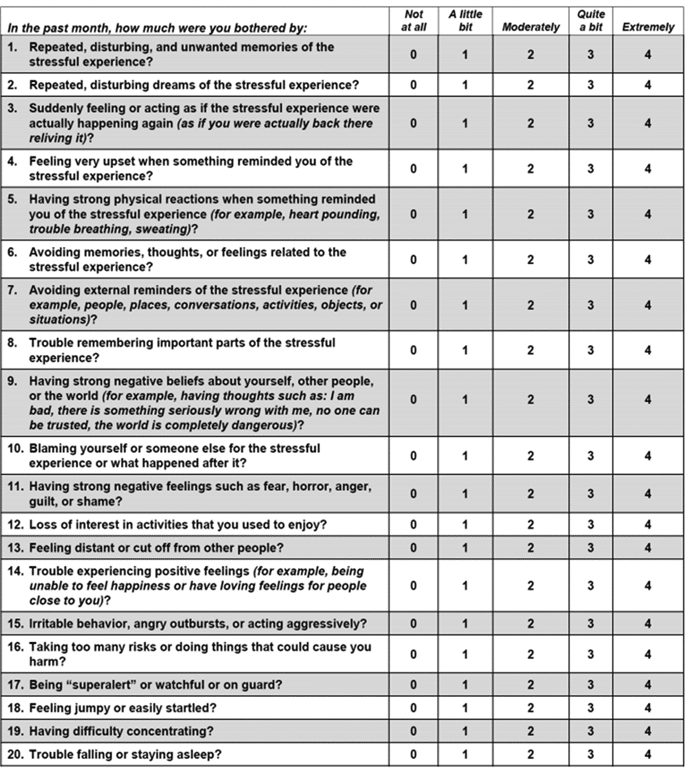
Ptsd: Screening & Assessment
is a 20-item self-report tool that corresponds to the 20 symptoms listed in DSM-5 . It can provide a global assessment of PTSD severity both at the time of diagnosis and over the course of treatment.
On a 4-point scale, scores can be tabulated for individual items to give information about the severity of the four DSM-5 symptom clusters. If a score of 2 is considered to be a positive endorsement of a given criterion, the PCL-5 can be used in combination with a clinical interview to make a provisional DSM-5 diagnosis. Testing the PCL-5 with veterans has determined a score of 31 to 33 to be a valid cutoff for a positive screen, but more work is necessary to validate this score in civilian populations .
Dissociative Experiences Scale
Because the DSM-5 incorporates a dissociative subtype of PTSD, it is useful to screen for dissociative symptoms, which are not captured by the PCL-5.
The self-report Dissociative Experiences Scale asks respondents to rate what percentage of the time they experience a given dissociative symptom . The general population average is 4 to 8 percent compared with 26 to 42 percent among people with PTSD . The DES cannot be used for diagnosis, but scoring over 20 per cent indicates the need to further explore dissociative symptoms .
The Posttraumatic Forensic Evaluation Of Minors
Now that the DSM-5 has supplanted the DSM-IV, evaluators must appropriately understand and use the new criteria, both in diagnosing and ruling out the presence of PTSD. Studies that used prototypes of the DSM-5 criteria demonstrated significant increases in the rates of diagnosis.,, By using the DSM-5 criteria, it is expected for several reasons that both the true incidence and true prevalence of PTSD will now increase for preschoolers. With the removal of the DSM-IV criterion A2 and an expansion of what constitutes a stressor for this age group, more children will now meet the threshold for criteria A. Symptoms of criteria B and C will be easier to detect, given the greater emphasis on the behavioral sequelae of trauma, as opposed to the former criteria, which required more verbal report. These symptoms can be observed by the evaluator and reported by collateral sources. The requirement for criteria C that only one symptom of avoidance or negative cognitions be present also removes what has been an obstacle in the past to application of the diagnosis to younger children: namely, so few children exhibited multiple symptoms in the domain of avoidance that it was very difficult for this age group to meet the full criteria.
Don’t Miss: How To Apply For Disability In Maryland
Chronic And Severe Ptsd
This section refers to research from PTSD resulting from a single trauma caused by physical or sexual assault/rape, rather than multiple traumas, although severe and persistent PTSD can be caused by either.Chronic PTSDAcute PTSD
- Nowhere is safe
- I cannot rely on other people
- I canât trust my own judgments
- It was my fault
Severe PTSDmild, moderate or severe,
- sense of hopelessness
- emotional detachment
initial
- See also: Complex PTSD for PTSD from multiple in erpersonal traumas, including child abuse
- See also: Treatment for PTSD, which includes a medication overview
- See also: PCL-5 PTSD checklist test to help assess PTSD
Suicide Risk And Comorbidities
Traumatic events increase a persons suicide risk, and PTSD is strongly associated with suicidal ideation and suicidal attempts.
PTSD is also linked to other mental disorders. According to DSM-5, those with PTSD are 80% more likely than those without it to have symptoms that meet the diagnostic criteria for at least one other mental disorder, such as depressive, bipolar, anxiety, or substance abuse disorders. Although females are at greater risk of PTSD, males diagnosed with PTSD are more likely to have a comorbidity. Among Afghanistan and Iraq veterans, its been found that the co-occurrence of PTSD and a mild traumatic brain injury was 48%.
Don’t Miss: Is Ptsd A Permanent Va Disability
What Is Complex Ptsd
It has long been recognised that the reactions of some people following traumatic events extend beyond previous definitions of PTSD . The DSM-5 took this into account with their wide approach as mentioned above. In contrast, the approach taken by ICD-11 was to formally define a new diagnosis of Complex PTSD. According to the ICD-11, Complex PTSD consists of the same core symptoms of PTSD, but has three additional groups of symptoms :
- Problems in affect regulation
- Beliefs about oneself as diminished, defeated or worthless, accompanied by feelings of shame, guilt or failure related to the traumatic event
- Difficulties in sustaining relationships and in feeling close to others
Research has indicated that the diagnosis of Complex PTSD can apply to children and young people. In one study, of those taking part in a treatment trial for PTSD, 40% of them had high levels of the additional symptoms required for Complex PTSD .
Criterion A: Exposure To Trauma

PTSD begins with criterion A, which requires exposure to a traumatic event. Criterion A is not only the most fundamental part of the nosology of PTSD, but also its most controversial aspect . Some trauma experts criticized criterion A in the DSM-IV as too inclusive and warned that this change had the potential to promote conceptual bracket creep or criterion creep . Some authors questioned the value of criterion A altogether , even suggesting that it should be abolished . Criterion A was retained in the DSM-5, but it was modified to restrict its inclusiveness.
Not all stressful events involve trauma. The DSM-5 definition of trauma requires actual or threatened death, serious injury, or sexual violence . Stressful events not involving an immediate threat to life or physical injury such as psychosocial stressors are not considered trauma in this definition.
Exposure to trauma is the foundation for the rest of the criteria that comprise the diagnosis of PTSD . Breslau et al. emphasized that the link between PTSD symptoms and exposure to a traumatic event is what makes the diagnosis of PTSD a distinct disorder. They posed the question, Without exposure to trauma, what is posttraumatic about the ensuing syndrome? . North et al. whimsically added that without exposure to trauma, a syndrome following a nontraumatic stressor might more appropriately be named poststressor stress disorder and one associated with no identified stressor called nonstressor stress disorder.
Read Also: Is Herniated Disc A Permanent Disability
